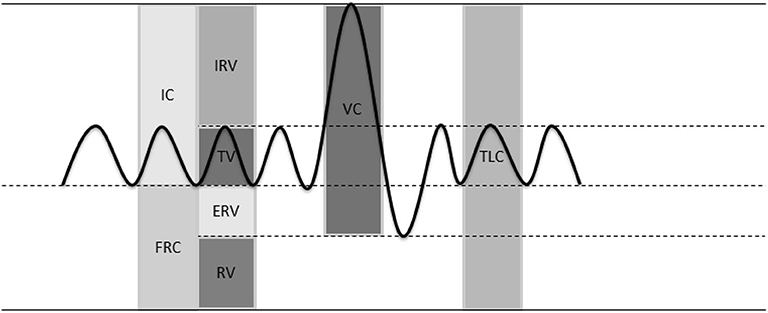
4– 6 Heulitt et al studied 68 infants and children to compare mVT using the Servo-i with aVT measured by a pneumotachometer placed between the Y-piece of the ventilator and the ETT. The majority of previous studies have reported that mVT overestimates aVT because of volume loss due to circuit compression. Many factors may lead to the dissociation between these parameters including volume loss when an uncuffed ETT is in use, circuit compression volume, and fresh gas flow. Our study revealed that there were clinically significant differences between sVT, mVT and aVT based on the severity of the simulated lung injury, the type of ventilator in use, as well as the mode of ventilation (VCV vs DCV). Furthermore, given variations in the technology and computer software, clinically significant differences may exist between the currently available ventilators. These issues may be magnified with smaller tidal volumes such as those used in neonates and in the presence of acute lung injury with changes in pulmonary resistance and compliance. Inaccuracies in the delivery of tidal volume may result in low minute ventilation and hypercarbia or excessive tidal volumes leading to barotrauma and lung injury. The accurate delivery of tidal volume is essential when ventilating neonates in both the ICU and during the intraoperative period. The tidal volume that was actually delivered to simulated neonatal patient (aVT) was measured by the syringe in ASL 5000 ( Figure 1). Ventilator displayed tidal volume hereafter referred to as measured tidal volume (mVT) was measured by the flow sensor in the expiratory limb of the ventilators. 
Each ventilator was evaluated using a respiratory rate of 25 breaths/minute, positive end-expiratory pressure (PEEP) 3 cmH2O, and an inspiratory time of 0.6 seconds in both the VCV and DCV modes. Set tidal volume (sVT) was 30 mL during all phases of the study. 3 After the standard initial machine check with a standard pediatric circuit, the ventilator was connected to the ASL 5000. 
Three lung models were set: resistance (cmH2O/L/sec) and compliance (mL/cmH2O) of 50, 2 (Group 1) 100, 1 (Group 2) and 150, 0.5 (Group 3) respectively, shown in Table 1. The lung simulator was used to simulate a 3 kilogram term neonate with and without lung involvement. Capnometer, heat moist exchanger, and humidifier were not connected to the circuit. The ASL 5000 was connected to a computer to analyze respiratory parameters and record tidal volumes. One anesthesia machine ventilator, Drager Fabius GS (Drager, Germany), and ICU ventilators including the Servo-i Universal™ version 3.0.1 (Maquet, Danvers, MA) and the Evita Infinity V500 (Drager, Lubeck, Germany) were evaluated. The ASL 5000 is a lung analogue, which can simulate various lung parameters (resistance and compliance) and precisely measure tidal volume. This lung simulation study was conducted using the Active Servo Lung 5000 (ASL 5000) (version 3.4, 3.5 IngMar Medical, Pittsburg, PA). This study was performed in Yokohama City University Hospital. 1 The aim of this study was to compare the set tidal volume (sVT) with the tidal volume measured by the ventilator (mVT), and the actual tidal volume (aVT) measured using a lung model to simulate neonatal anesthesia care. However, now that cuffed ETTs have become more common in clinical care, it may be feasible to use VCV and DCV in neonates. These factors may be magnified with the variable leak when an uncuffed ETT is used. PCV has been the mainstay of mechanical ventilation in neonates because of concerns of inaccurate tidal volume related to fresh gas flow, circuit compression volume, circuit compression volume, and changing resistance and compliance. DCV is also referred to as volume-targeted ventilation, pressure-regulated volume-controlled ventilation (PRVC), and pressure-controlled ventilation with volume guarantee (PCV-VG). DCV is an auto-regulated mode of pressure-controlled ventilation that achieves a set tidal volume. Modern-day ventilators on the anesthesia machine have volume-controlled ventilation (VCV), pressure-controlled ventilation (PCV), and dual-controlled ventilation (DCV). The efficacy of such software has been previously demonstrated with tidal volumes as low as 100 mL. Specific computer software has been developed to allow the ventilator to compensate for the volume loss within the circuit. Discrepancies between the set and actual delivered tidal volume can result from various factors including circuit compression volume and the impact of fresh gas flow. 1 Tidal volume (VT) is usually measured by a sensor placed at the expiratory valve or within the expiratory limb of the ventilator. Precise control of tidal volume is one of the keys in limiting ventilator-induced lung injury (VILI), ensuring adequate ventilation, and improving outcomes in mechanically ventilated neonates.
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
